Knee surgeries in athletes
Sports injuries of the knee
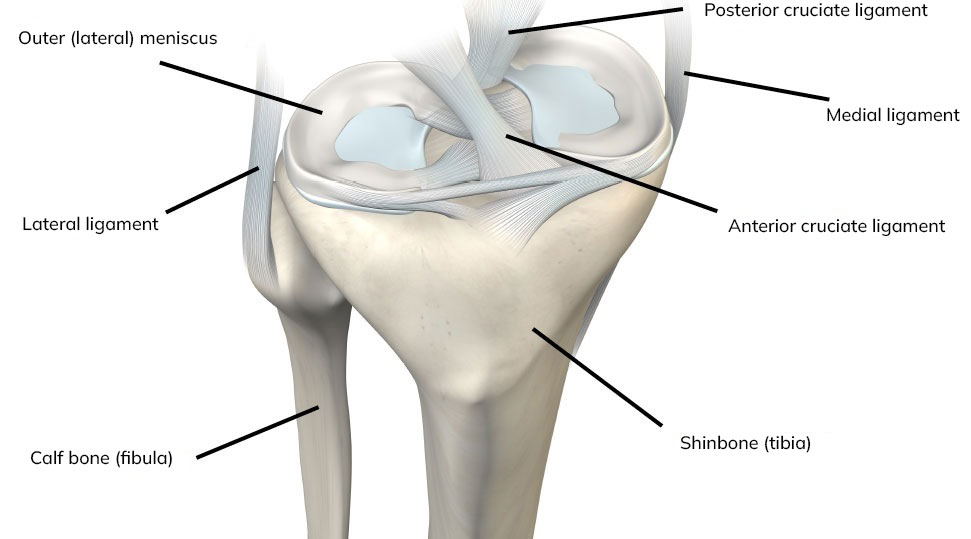
Torn anterior cruciate ligament (ACL)
The anterior cruciate ligament (ACL) is located in the center of the knee and plays a crucial role in knee stability. It prevents the shinbone from moving forward and rotating in relation to the thigh bone. Sports that involve cutting and pivoting movements, such as soccer, hockey, tennis, and handball, require this stability. Approximately 70% of ACL tears occur when a sudden twisting motion or improper landing happens during sports activities. The remaining 30% result from collisions with other players.
Symptoms of a torn ACL include:
- A popping sensation or sound at the time of injury
- Swelling of the knee
- Instability
- Pain
Treatment of a torn ACL in (elite) athletes
The initial step in treatment is to reduce knee swelling and restore knee function, particularly flexion and extension. An MRI scan is typically performed to assess any associated injuries.
If you and your surgeon decide to proceed with surgery, the torn ACL will be replaced with one of the following tendons:
- Hamstring tendons
- Patellar tendon
- Quadriceps tendon
The choice of tendon depends on factors such as other knee injuries, the degree of knee instability, the sport you participate in, and the level at which you compete.
Lateral tenodesis - Lemaire plastic surgery
Although anterior cruciate ligament (ACL) reconstruction is a successful surgery, the new ACL can tear again. The reasons for this are multifactorial. Factors such as re-injury or twisting of the knee, patient age, and gender can play a role. Specific characteristics of the knee also influence the risk of re-tearing, such as the ability to hyperextend the knee.
As mentioned above, one of the important functions of the ACL is to prevent inward rotation of the lower leg in relation to the upper leg. The ACL, together with the structures on the outer side of the knee, helps to prevent this rotation. If these structures on the outer side of the knee are not addressed during the ACL surgery, the new ACL can tear again.
The surgical treatment of these structures on the outer side of the knee is called lateral tenodesis, also known as Lemaire plastic surgery. During this procedure, an additional reinforcement is created between the tibia and femur on the outer side of the knee. The image shows how a portion of your own tendon (the iliotibial tract) is used on the outer side of the knee to create a connection and reinforcement between the tibia and femur. Recent studies have shown that when the tenodesis is performed together with ACL reconstruction, there is a 64% lower chance of re-tearing the reconstructed ACL.
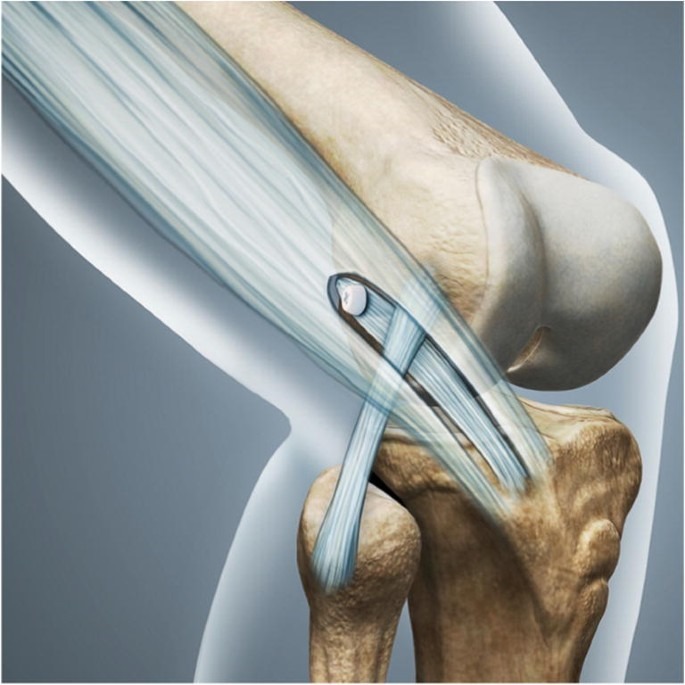
Indications for a lateral tenodesis
Not everyone requires this surgery, and it is primarily recommended for patients who are at high risk of re-tearing their anterior cruciate ligament (ACL):
- Patients with hyperlaxity/hypermobility
- Patients younger than 20-25 years
- Revisions of a previously performed
- ACL reconstruction
- Elite athletes participating in cutting and pivoting sports such as football, hockey, tennis, and handball.
Are there any disadvantages of a lateral tenodesis?
Performing a lateral tenodesis extends the standard scar on the outer side of the knee from 2cm to 3 to 4 cm. In the first 6 weeks after the surgery, there may be slightly more pain on the outside of the knee. However, after this period, there is no difference compared to an ACL reconstruction without tenodesis.
A torn medial collateral ligament (MCL) of the knee.
If you tear your MCL, your orthopedic surgeon will assess the degree of instability and the location of the tear. Grade I injuries involve only pain without instability, and they typically heal on their own within 4 to 6 weeks. Grade II injuries involve a partial tear with moderate instability. Grade III injuries involve a complete tear of the MCL.
If diagnosed promptly, grade II and III injuries can be effectively treated with a brace. However, if brace treatment is initiated several weeks after the injury, the outcomes are typically poorer. If instability persists, surgery may be considered, in which the MCL can be repaired and reinforced using your own hamstring tendons. This procedure is known as an MCL reconstruction.
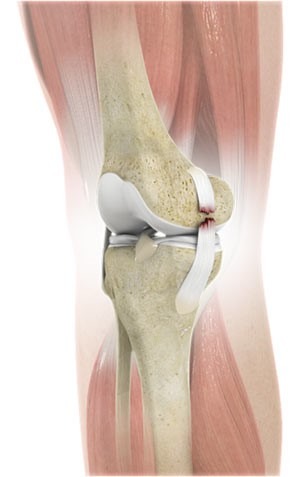
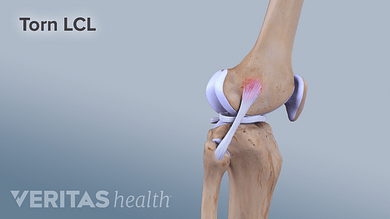
A torn lateral collateral ligament (LCL) of the knee
The diagnosis is made during the physical examination. In all cases, an MRI scan is performed.
Similar to the treatment for a torn medial collateral ligament, the treatment for a torn lateral collateral ligament depends on the degree of instability and the timing of the diagnosis. If the injury is 1-2 weeks old, it can be effectively treated with a brace or cast. However, if the injury is older, brace treatments are less successful. If instability prevents sports activities, surgery may be necessary. The type of surgery depends on the alignment of the leg (varus or valgus) and the presence of any additional knee damage. Examples of surgeries commonly performed for a torn lateral collateral ligament with instability include a reconstruction of the lateral ligaments or a corrective osteotomy, also known as a posterolateral corner reconstruction.
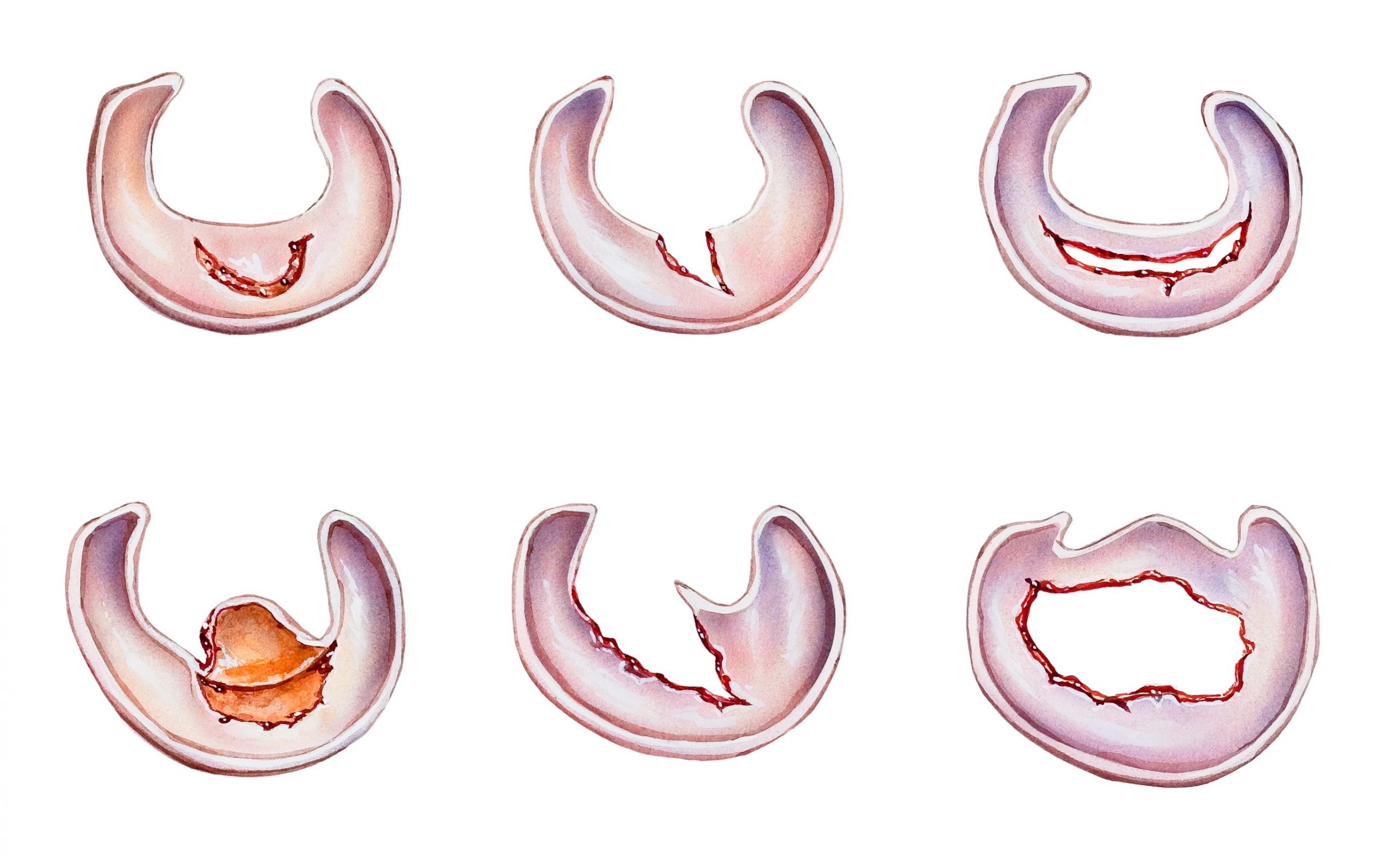
A torn meniscus
A torn meniscus is the result of damage to the shock-absorbing cartilage in the knee. There are two menisci in the knee, the medial meniscus on the inside and the lateral meniscus on the outside. Twisting the knee during sports activities can cause a meniscus tear, often accompanied by damage to the knee ligaments.
Symptoms of a torn meniscus include:
- Pain and swelling in the knee
- Feeling a clicking sensation in the knee
- In severe cases, the knee may become locked, preventing full extension and flexion (known as a “locked knee”)
- Instability and lack of confidence in the knee
The diagnosis is made during a physical examination at the outpatient clinic. An MRI scan is typically performed to assess the location and type of tear and to obtain a comprehensive view of the knee.
Depending on the type of tear and the symptoms experienced, a decision will be made whether or not to proceed with surgery. Non-operative treatment options include a course of anti-inflammatory medication (NSAIDs) and physiotherapy. However, not all tears can be treated conservatively. In such cases, a knee arthroscopy, also known as a “keyhole surgery,” may be performed. This involves making two small incisions in the front of the knee to visualize the entire joint and address the torn meniscus. In some cases, a small portion of the torn meniscus may be removed (meniscectomy). However, whenever possible, the goal is to repair the torn meniscus (meniscopexy). The decision regarding the appropriate treatment approach will be made during the surgery.